Obesity
GLP-1s (it’s kind of a mess)
“But the real question is what is the quality of the weight regain and what is the shift in people’s metabolism, and it seems to be very bad,” she said. “Ongoing studies that haven’t been published yet suggest that hypertension comes back. All the inflammatory markers come back, and lipids go up. And if you have diabetes, it gets worse. Overall, it’s kind of a mess…As these studies and others showed, most people regain the weight. Whether or not they regain all the weight depends in part on diabetes and insulin and many other factors, but people will likely regain most of their weight.”
“But the message isn’t that you regain the weight. The message is that you may be less healthy when you regain the weight. That’s why we need to couple the drugs with lifestyle interventions. And it’s why people who just want to lose 5 or 10 pounds really need to consider that lifestyle change, hard as it is, is the better way to do it.”
Anne Peters, MD, professor Keck School of Medicine of the University of Southern California
Less Weight Regain, More Health Loss after Stopping GLP-1s? – Medscape – March 05, 2026 – https://www.medscape.com/viewarticle/less-weight-regain-more-health-loss-after-stopping-glp-1s-2026a10006rv?
I never envisioned developing an obsession with pharmaceuticals. And after many years of endless blogging into the void I learned I could link to previous posts like this: https://lifeunderwriter.net/tag/glp-1-receptor-agonist/
The learning never stops.
Medscape on Obesity – 02.08.26
GLP-1s and the Risk for Malnutrition
“We see cases where people take a GLP-1 medication and become so severely malnourished that they need to be hospitalized,” said Rebecca Boswell, PhD, director of Penn Medicine Princeton Center for Eating Disorders, in Philadelphia. “It’s not uncommon.” The Scary Health Risk That Can Sneak Up on GLP-1 Users – Medscape – January 19, 2026. https://www.medscape.com/viewarticle/scary-health-risk-can-sneak-glp-1-users-2026a10001pi
Yikes.
People return to their baseline weight and lose all cardiometabolic benefits in less than 2 years after stopping semaglutide or tirzepatide, a new meta-analysis found. Weight Regain, Health Benefit Loss Rapid When GLP-1s Stopped – Medscape – January 08, 2026. https://www.medscape.com/viewarticle/weight-regain-health-benefit-loss-rapid-when-glp-1s-stopped-2026a10000kr?
YIKES.
You see, cures are passée. Cures kill markets. Getting the population properly hooked on a pharmaceutical treatment for a ‘chronic’ condition is where the serious money is. “Our core insight was simple and grim: it’s far easier—and infinitely more profitable—to convince healthy people that they’re sick than to develop genuine cures for the truly ill.“
Twenty years later, the hustle is bigger, slicker, and more dangerous than ever. Watching that hustle unfold with weight loss drugs feels weirdly ominous, like watching a slow-moving train wreck you can’t peel your eyes off of. You know there’ll be carnage and bodies, vast fortunes won and lost, and humanity left just a little bit poorer. We have often documented the pharmaceutical industry’s proven ability to create enormously lucrative markets overnight, by inventing and selling diseases. Now watch as all that ingenuity and energy gets pointed at one of the biggest problems bewitching humanity: human fatness. The Seven Deadly Sins of Weight Loss Drugs – https://brownstone.org/articles/the-seven-deadly-sins-of-weight-loss-drugs/
YIKES!
This will not end well.
Complications? What Complications? (just another GLP-1 receptor agonist post)
PATHWEIGH Weight Management Model
The power of PATHWEIGH is that it puts patients and their primary care provider on the same page…It all started with signage placed in clinics that notified patients that if they wanted to make an appointment to specifically talk about weight management, all they had to do was approach the desk and ask for it. That request automatically triggered a mechanism in the patient’s electronic health record that sent them a survey that after completion would flow into the provider’s notes. Instead of spending so much time typing and talking about the patient’s history, the scheduled visit could be centered around solutions. PATHWEIGH: A Model Changing Weight Management For All – https://news.cuanschutz.edu/medicine/pathweigh-pilot-research
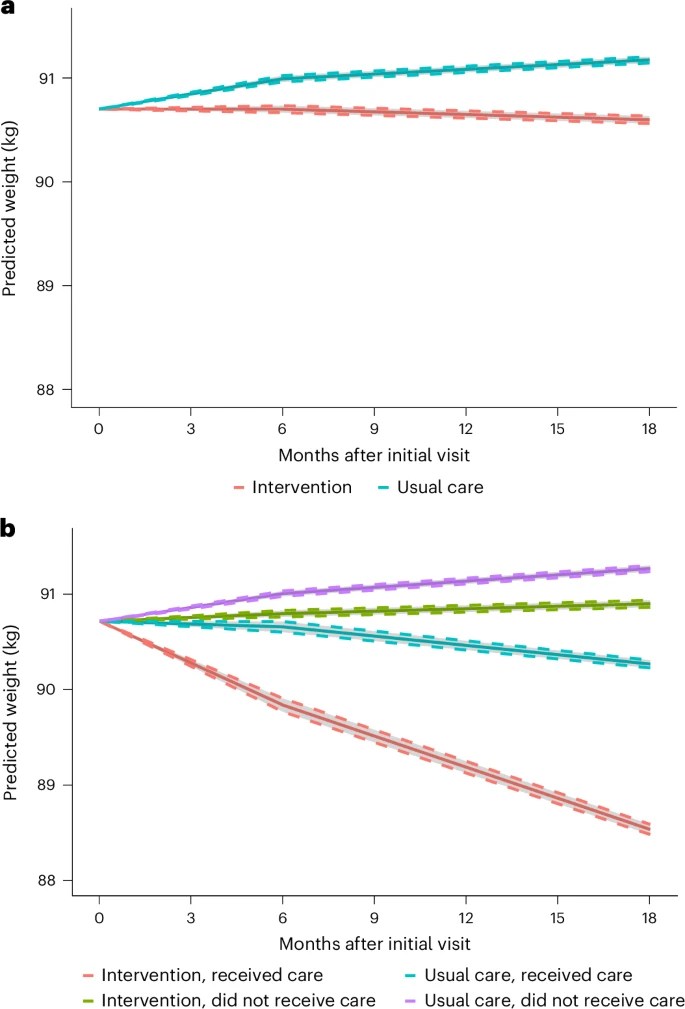
Implementation and effectiveness of a care process to prioritize weight management in primary care: a stepped-wedge cluster-randomized trial – https://www.nature.com/articles/s41591-025-04051-5#Sec1
Medscape 2025 Obesity Articles
But I Lost 20 Pounds!
There have been hundreds of reports of acute and chronic pancreatitis from people who have taken drugs such as Mounjaro, Ozempic and Wegovy, although none are confirmed as being caused by the medicines. Weight loss jabs study begins after reports of pancreas issues – https://www.bbc.com/news/articles/c4ged0r1n3wo
Yikes.
Child Obesity Clinics in England Seeing BMIs over 50
Read article at this link https://www.bbc.com/news/articles/cvg7w58yddgo
Yikes!
What Really Works for Long-Term Weight Loss
From diet to drugs: what really works for long-term weight loss
Ultimately, the key to lasting weight loss and improved health lies in understanding that there is no one-size-fits-all solution. It’s about finding the right combination of support, strategy and science that works for each person. Reiner Jumpertz-von Schwartzenberg – Professorship for Clinical Metabolism and Obesity Research, University Hospital and Medical Faculty, University of Tübingen – https://theconversation.com/from-diet-to-drugs-what-really-works-for-long-term-weight-loss-254551
I read the entire article so you don’t have to. You’re welcome.
Well, knowing there is NO one-size-fits-all changes my future best selling book on weight loss drastically.
What was a “how to” is now memoir. Sigh.
Obesity is Not a Disease
David L. Katz, MD, MPH, FACPM, FACP, FACLM is a specialist in Internal Medicine, Preventive Medicine/Public Health, and Lifestyle Medicine – globally recognized for expertise in chronic disease prevention, health promotion, and nutrition. The founding director of Yale University’s Prevention Research Center, and past president of the American College of Lifestyle Medicine, Katz is the founder of the non-profit True Health Initiative, founder of Diet ID, and Chief Medical Officer for leading food-as-medicine company, Tangelo. He is a senior science advisor to Blue Zones. He holds multiple US patents, including for advances in dietary assessment. He has roughly 250 peer-reviewed publications, has authored 19 books- including multiple editions of a leading textbooks in nutrition and preventive medicine, and has earned numerous awards for his contributions to public health, including three honorary doctoral degrees.
https://www.vumedi.com/video/obesity-is-not-a-disease-so-what-is-it
Diet until proven otherwise.
You must be logged in to post a comment.