Seven mutations appeared in a strain of H3N2 seasonal flu and led to a “fast increase” in reports of the mutated virus, says Prof Derek Smith, director of the centre for pathogen evolution at the University of Cambridge. New flu virus mutation could see ‘worst season in a decade’ https://www.bbc.com/news/articles/c2dr8gzdz1wo
Infectious Diseases
Not Just For Allergic Rhinitis Anymore
A common hay fever nasal spray was found to cut COVID-19 infections by two-thirds in a clinical trial, while also reducing rhinovirus cases. Researchers believe it could serve as an easy, low-cost preventive measure, pending further studies. Saarland University. “Common allergy spray slashes COVID-19 risk in surprising trial.” ScienceDaily. http://www.sciencedaily.com/releases/2025/09/250907024535.htm (accessed September 7, 2025).
For Robert Bals, the results suggest practical applications: ‘Azelastine nasal spray could provide an additional easily accessible prophylactic to complement existing protective measures, especially for vulnerable groups, during periods of high infection rates, or before travelling.’ But Professor Bals also stressed the importance of further research: ‘Our results highlight the need for larger, multicentre trials to continue exploring the use of azelastine nasal sprays as an on-demand preventive treatment, and to examine its potential effectiveness against other respiratory pathogens.’
Link to the Jama article – https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/2838335 Azelastine Nasal Spray for Prevention of SARS-CoV-2 Infections
Bartonella henselae?
The case study that caught my attention involved a 26-year-old woman who had experienced mild COVID-19 but continued to suffer from persistent symptoms for five months afterward, including noticeable axillary (armpit) lymph node swelling. When doctors performed a biopsy of the swollen lymph node and analyzed it with clinical metagenomic testing, they discovered something unexpected: Bartonella henselae DNA and RNA. Even more telling was that when the patient was treated with the antibiotic clarithromycin, her symptoms improved.
This case illustrates something I’ve suspected and observed in my practice: COVID-19 may be reactivating latent infections that were previously dormant in the body. The immune dysregulation caused by SARS-CoV-2 appears to create an environment where opportunistic pathogens like Bartonella can resurface and cause symptoms. Hidden Infections Behind Long COVID: Unmasking Bartonella henselae – https://www.jillcarnahan.com/2025/06/21/hidden-infections-behind-long-covid-unmasking-bartonella-henselae/
Hmm… https://www.cdc.gov/bartonella/about/about-bartonella-henselae.html
Enjoy Your Cruise (avoid the hot tub)
Legionnaires disease is a serious pneumonia caused by Legionella bacteria. Hot tubs can be a source of Legionella growth and transmission when they are inadequately maintained and operated. Private hot tubs on cruise ships are not subject to the same maintenance requirements as are public hot tubs in common areas. Lee S, Edens C, Ritter T, et al. Two Outbreaks of Legionnaires Disease Associated with Outdoor Hot Tubs for Private Use — Two Cruise Ships, November 2022–July 2024. MMWR Morb Mortal Wkly Rep 2024;73:950–954. DOI: http://dx.doi.org/10.15585/mmwr.mm7342a3
Plant Based Diets and Covid-19
Of the total participants, 47 percent reported having had COVID-19 infection. The omnivorous group had a significantly higher incidence of infection (52 percent vs. 40 percent) and were more likely to experience moderate to severe symptoms (18 percent vs. 11 percent).
After adjusting for influential factors such as weight, pre-existing medical conditions, and physical activity levels, there was no overall difference in symptom severity between the groups. However, those following predominantly plant-based or vegetarian diets were 39-percent less likely to become infected than their omnivorous counterparts.
The researchers suggest that plant-based diets may contribute to a boosted immune system and better defense against viral infections due to their richness in antioxidants, phytosterols, and polyphenols.
Plant-Based Diets Linked to 39 Percent Lower COVID-19 Infection Rate, Study Finds — https://vegnews.com/vegan-news/plant-based-diet-low-covid-19-infection-rate-study
Link to the original study Vegetarian and plant-based diets associated with lower incidence of COVID-19 — https://nutrition.bmj.com/content/early/2024/01/02/bmjnph-2023-000629
Eat more plants.
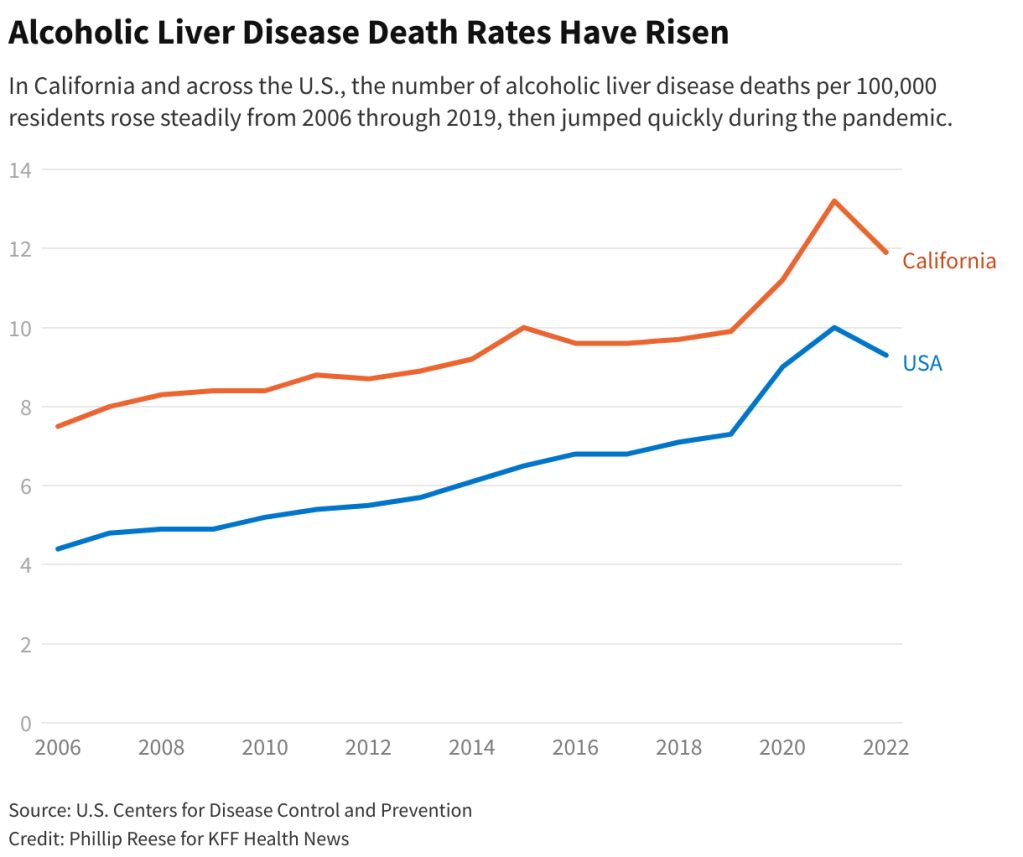
Scary Charts – 07.16.23
Note the Pandemic Bump. Overall trend lines for both CA and USA still heading north.
CA only. USA death rates probably show a similar pattern.
CA statistics. NOTE the ASIAN RATE.
Excessive drinking during the covid-19 pandemic increased alcoholic liver disease deaths so much that the condition killed more Californians than car accidents or breast cancer, a KFF Health News analysis has found. Lockdowns made people feel isolated, depressed, and anxious, leading some to increase their alcohol intake. Alcohol sales rose during the pandemic, with especially large jumps in the consumption of spirits.
Excessive Drinking During the Pandemic Increased Alcoholic Liver Disease Death Rates — https://kffhealthnews.org/news/article/excessive-drinking-during-the-pandemic-increased-alcoholic-liver-disease-death-rates/
Yes it’s Sunday morning and I’m thinking about single malt Scotch because I ran out.
Take Home Lesson for UW Professionals
The highest mortality rates were Gen X and Boomers.
Memo to Self
Think before you drink.
Answers emerge about long COVID recovery – Nature Briefing
How many people with long COVID recover
Research is slowly shedding light on how many people get bettter from long COVID, despite debate over the definition of the condition, its cause and what ‘recovery’ even means. Improvements seem to plateau after one year: in a study of 1,106 people, close to 23% still had symptoms after six months, falling to around 19% after one year and 17% after two. Another study finds that one-third of people who had symptoms after six months no longer had them at nine months. Risk factors include being female, being older, having a high body mass index, smoking, having asthma or diabetes, and having a severe COVID-19 infection. Vaccination seems to reduce the risk. The diabetes drug metformin and the antiviral Paxlovid are showing promise for preventing long COVID — but only if given during the acute phase.
Daily briefing: Answers emerge about long COVID recovery – https://www.nature.com/articles/d41586-023-02190-8
Yikes!
Common Cold May Give Children Immunity against COVID-19 — Wellness Secrets of a SuperAger

During the pandemic, medical doctors and researchers noticed that children and adolescents infected with COVID-19 became less ill than adults. A possible explanation for this is that children already had a prior level of immunity to COVID-19 provided by memory T cells generated by common colds. Photo by Pixabay on Pexels.com After studying unique blood […]
Common cold gives children immunity against COVID-19 — Wellness Secrets of a SuperAger
Thanks Tony. Good stuff. Small sample size and more research is needed on this topic.
Outbreak Linked to Eyedrops
An alarming outbreak of extensively drug-resistant bacteria linked to eye drops has now sickened 68 people across 16 states, according to the latest update from the Centers for Disease Control and Prevention. At least 16 people have been hospitalized, eight have lost vision, and four have had their eyeballs surgically removed (enucleation). One person has died, which was reported earlier.
The VIM-GES-CRPA outbreak strain is rare and has never been seen in the US before. Health officials think it was brought into the country in contaminated eye drops manufactured by Global Pharma, a Chennai, India-based manufacturer. The products were sold under the brand names EzriCare Artificial Tears and Delsam Pharma’s Artificial Eye Ointment, which were available nationwide via Amazon, Walmart, and other retailers.
68 now sickened, 4 lose eyeballs in outbreak linked to eyedrops — https://arstechnica.com/science/2023/03/more-people-lose-eyeballs-in-outbreak-linked-to-eye-drops/
Yikes!
Unhealthful Eating – Pandemic Style
Mindless eating and snacking;
Increased food consumption;
Generalized decrease in appetite or dietary intake;
Eating to cope;
Pandemic-related reductions in dietary intake;
And, a re-emergence or marked increase in eating disorder symptoms.
Approximately 8% of those studied reported extreme unhealthy weight control behaviors, 53% had less extreme unhealthy weight control behaviors and 14% reported binge eating. The study revealed that these outcomes were significantly associated with poorer stress management, greater depressive symptoms and moderate or extreme financial difficulties.
University of Minnesota Medical School. “COVID-19 pandemic has been linked with six unhealthy eating behaviors: Study shows a slight increase in eating disorders, one of the deadliest psychiatric health concerns.” ScienceDaily. http://www.sciencedaily.com/releases/2021/04/210412114740.htm (accessed May 1, 2021).
Pandemic or no pandemic at times I am guilty of number one on the list. I found the absolute best pita crackers, crispy and salty, and…




You must be logged in to post a comment.