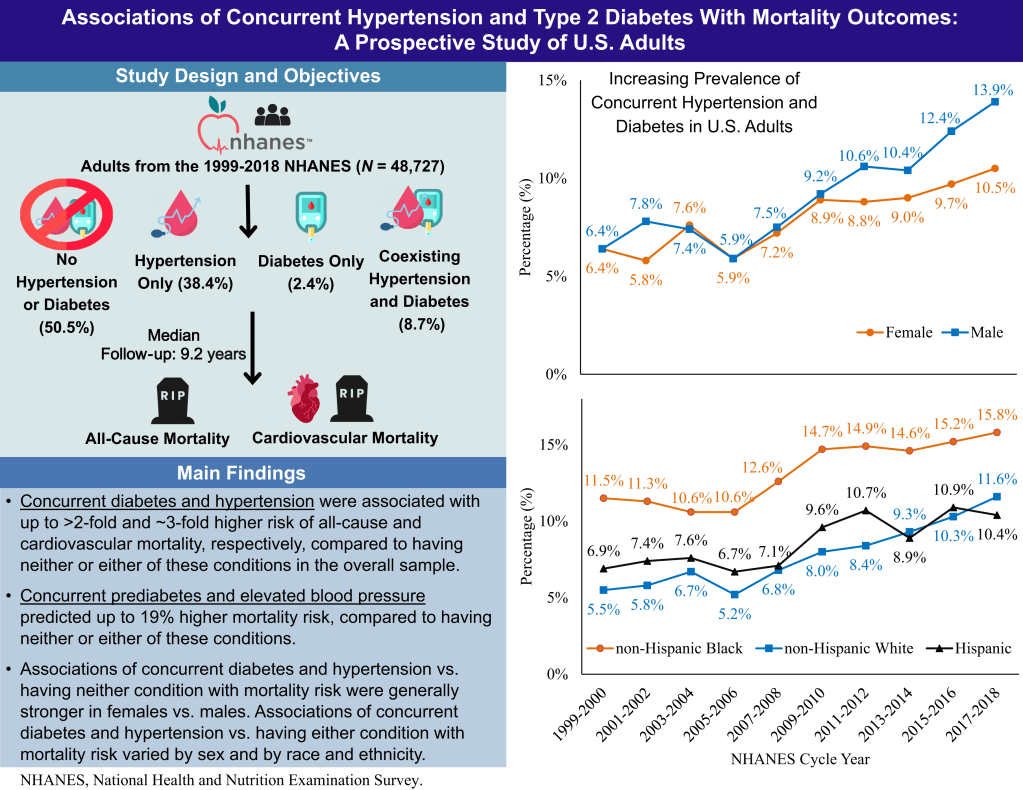
Associations of Concurrent Hypertension and Type 2 Diabetes With Mortality Outcomes: A Prospective Study of U.S. Adults – Diabetes Care 2025;48(7):1241–1250 https://doi.org/10.2337/dca24-0118
Hypertension
Just 2-4 Cups of Fruits and Veggies Does What?
Lowers blood pressure, improves kidney health, improves CVD risk factors.
In a randomized control trial over a five-year period, investigators divided the cohort of 153 patients with hypertension into three groups:
- Study participants adding 2-4 cups of base-producing fruits and vegetables in addition to their usual daily food intake
- Study participants prescribed NaHCO3 (acid-reducing sodium bicarbonate, which is common baking soda) tablets in two daily doses of 4-5 650 mg tablets
- Study participants receiving standard medical care from primary care clinicians
The results of the study show that both fruits and vegetables and NaHCO3 improved kidney health, but only fruits and vegetables, and not NaHCO3, reduced blood pressure and improved indices of cardiovascular disease risk.
The trial supports fruits and vegetables as foundational hypertension treatment to reduce chronic kidney disease progression and cardiovascular disease risk.
Elsevier. “Eating more fruits and vegetables to reduce dietary acid lowers blood pressure and improves kidney and heart health in patients with hypertension.” ScienceDaily. http://www.sciencedaily.com/releases/2024/08/240806131316.htm (accessed August 11, 2024).
Journal Reference:
- Nimrit Goraya, Nicolaos E. Madias, Jan Simoni, Maninder Kahlon, Nazan Aksan, Donald E. Wesson. Kidney and Cardiovascular Protection Using Dietary Acid Reduction in Primary Hypertension: A Five-Year, Interventional, Randomized, Control Trial. The American Journal of Medicine, 2024; DOI: 10.1016/j.amjmed.2024.06.006
I had two cups of fruit in my breakfast bowl this morning.
What did you eat for breakfast?
Just Another Sweet Saturday Morning
These findings show that the prevalence of food insecurity in the U.S. is highest among Americans for whom a healthy diet is especially critical—Medicaid enrollees with insulin-dependent diabetes and diabetes-related eye or kidney complications (over 40% were food insecure). The problem of co-occurring food insecurity and diabetes among the nation’s disadvantaged has likely worsened during the coronavirus disease 2019 pandemic.
The Prevalence of Food Insecurity Is Highest Among Americans for Whom Diet Is Most Critical to Health — Diabetes Care 2021 Jun; 44(6): e131-e132. https://doi.org/10.2337/dc20-3116
In patients with newly diagnosed T2DM, alcohol abstinence was associated with a low risk of AF development. Lifestyle modifications, such as alcohol abstinence, in patients newly diagnosed with T2DM should be recommended to reduce the risk of AF.
Diabetes Care 2021 Jun; 44(6): 1393-1401. https://doi.org/10.2337/dc20-2607
New research published in Diabetologia has shown that if people achieve and maintain substantial weight loss to manage their type 2 diabetes, many can also effectively control their high blood pressure and stop or cut down on their anti-hypertensive medication.
Diabetologia. “Diabetes remission diet also lowers blood pressure and reduces need for medication.” ScienceDaily. ScienceDaily, 31 May 2021 — https://www.sciencedaily.com/releases/2021/05/210531180422.htm
Sat 6/19
Spice Blend
1 teaspoon ground cumin
1 teaspoon ground coriander
1 teaspoon smoked paprika
½ teaspoon ground turmeric
½ teaspoon dried oregano
½ teaspoon dried chili flakes
¼ teaspoon ground cinnamon
Copied from The First Mess Seven Spice Chickpea Stew recipe https://thefirstmess.com/2016/01/20/vegan-seven-spice-chickpea-stew-recipe/ so I don’t have to look it up online again if I decide to make this dish tonight.
During Pandemic Year One I lost 25 pounds. My PCP was impressed but when I told her how my diet changed she put her “doctor face” on, looked me straight in the eyes and said,
“I can’t wait to see your blood test results.”
Due to my family history my risk of developing DM2 is approximately 25% higher than the average underwriter. When I asked a prominent Endocrinologist for some advice many years ago he too put on his “doctor face” looked me straight in the eyes and said,
“Stay as thin as you can as long as you can.”
Yesterday I went to see Kevin and got a fresh flattop. The first question he asked was,
“Did you lose more weight?”
No, I haven’t. But my face definitely looks thinner without a mask.

BTW my blood work was about the same as last year even with my change in diet.
Preferred Plus NN.
Cardiovascular Events and Mortality in White Coat Hypertension: A Systematic Review and Meta-analysis
Limitation: Paucity of studies evaluating isolated cardiac outcomes or reporting participant race/ethnicity. Conclusion: Untreated WCH, but not treated WCE, is associated with an increased risk for cardiovascular events and all-cause mortality. Out-of-office BP monitoring is critical in the diagnosis and management of hypertension.
Vital Signs: Disparities in Antihypertensive Medication Nonadherence Among Medicare Part D Beneficiaries — United States, 2014 – MMWR
 Source: Vital Signs: Disparities in Antihypertensive Medication Nonadherence Among Medicare Part D Beneficiaries — United States, 2014 | MMWR
Source: Vital Signs: Disparities in Antihypertensive Medication Nonadherence Among Medicare Part D Beneficiaries — United States, 2014 | MMWR
Conclusions and Implications for Public Health Practice:
More than one in four Medicare Part D beneficiaries using anti-hypertensives were non-adherent to their regimen, and certain racial/ethnic groups, states, and geographic areas were at increased risk for non-adherence.
Blood pressure variability and cardiovascular disease: systematic review and meta-analysis – The BMJ
Results – 41 papers representing 19 observational cohort studies and 17 clinical trial cohorts, comprising 46 separate analyses were identified. Long term variability in blood pressure was studied in 24 papers, mid-term in four, and short-term in 15 (two studied both long term and short term variability). Results from 23 analyses were excluded from main analyses owing to high risks of confounding. Increased long term variability in systolic blood pressure was associated with risk of all cause mortality (hazard ratio 1.15, 95% confidence interval 1.09 to 1.22), cardiovascular disease mortality (1.18, 1.09 to 1.28), cardiovascular disease events (1.18, 1.07 to 1.30), coronary heart disease (1.10, 1.04 to 1.16), and stroke (1.15, 1.04 to 1.27). Increased mid-term and short term variability in daytime systolic blood pressure were also associated with all cause mortality (1.15, 1.06 to 1.26 and 1.10, 1.04 to 1.16, respectively).
Conclusions – Long term variability in blood pressure is associated with cardiovascular and mortality outcomes, over and above the effect of mean blood pressure. Associations are similar in magnitude to those of cholesterol measures with cardiovascular disease. Limited data for mid-term and short term variability showed similar associations. Future work should focus on the clinical implications of assessment of variability in blood pressure and avoid the common confounding pitfalls observed to date.
Source: Blood pressure variability and cardiovascular disease: systematic review and meta-analysis | The BMJ
Blood Pressure and Complications in DM2 and no Previous CVD – The BMJ
Conclusions: Lower systolic blood pressure than currently recommended is associated with significantly lower risk of cardiovascular events in patients with type 2 diabetes. The association between low blood pressure and increased mortality could be due to concomitant disease rather than anti-hypertensive treatment.
Intensive Tx Fails to Slow Atherosclerosis | Medpage Today
“When we see something that surprises us and flies in the face of what is understood, it requires another look — maybe a different cohort, larger numbers, longer follow-up,”
via Intensive Tx Fails to Slow Atherosclerosis | Medpage Today.
Surprised? As long as we continue to focus on pharmaceuticals as the answer, no one should be surprised.
Hypertension Becoming More Deadly? – Medpage Today
Hypertension is increasingly contributing to U.S. mortality, a national death-certificate study showed.
Low Vitamin D Causes High BP
Note that this large genetic analysis demonstrated that individuals with genes linked to lower vitamin D levels are more likely to have hypertension mediated by low vitamin D, strengthening the argument for a causal link.
Be aware that the absolute effect of vitamin D levels on blood pressure was negligible, even though statistically significant.
You must be logged in to post a comment.