In the journal Nature Medicine this week there was an important open-access publication about a large combined cohort of over 105,000 health professionals prospectively followed for 30 years. Only 9.3% reached the age of 70 years with “healthy aging” —without 11 major chronic diseases and no impairment of cognitive or physical function or mental health. Our Diet and Healthy Aging Eric Topol, MD – https://erictopol.substack.com/p/our-diet-and-healthy-aging
Dr. Eric Topol’s assessment of this study is well balanced and thoughtfully written. His bio is here: https://www.scripps.edu/faculty/topol/
Healthy aging in this study is described as reaching age 70 without developing any of 11 major diseases: cancer (except for non-melanoma skin cancers), diabetes, heart attack, coronary artery disease, congestive heart failure, stroke, kidney failure, chronic obstructive pulmonary disease, Parkinson disease, multiple sclerosis and amyotrophic lateral sclerosis.
My Half-Birthday is coming up soon. I’ll be 70.5 years young. The biggest take home lesson for me is this:
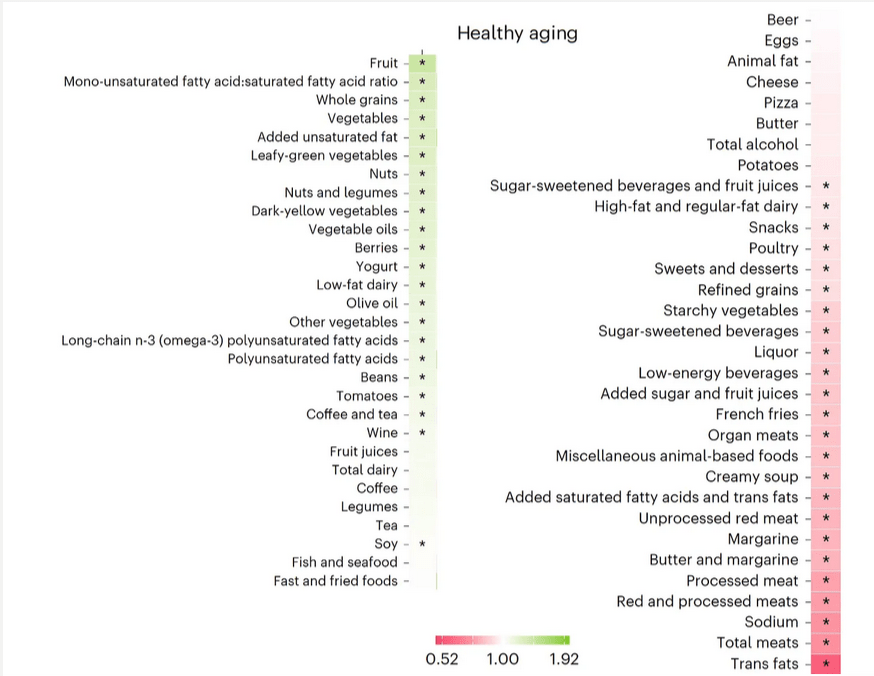
Beer is better for you than pizza.
You must be logged in to post a comment.