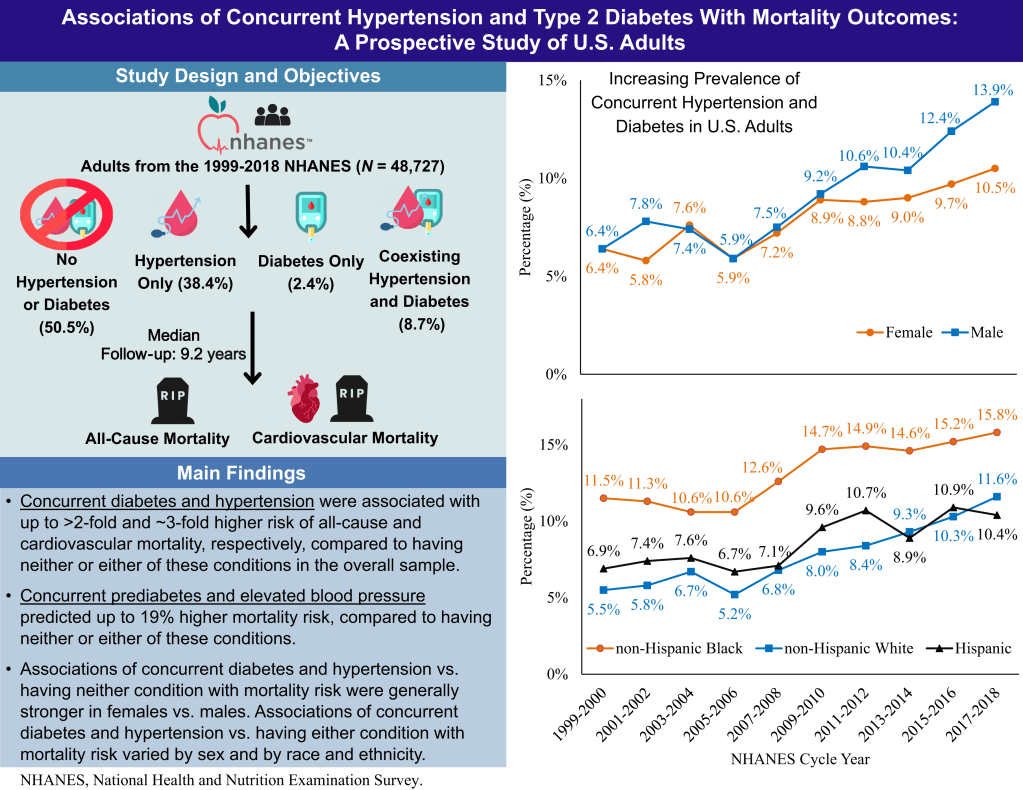
Associations of Concurrent Hypertension and Type 2 Diabetes With Mortality Outcomes: A Prospective Study of U.S. Adults – Diabetes Care 2025;48(7):1241–1250 https://doi.org/10.2337/dca24-0118
life underwriting
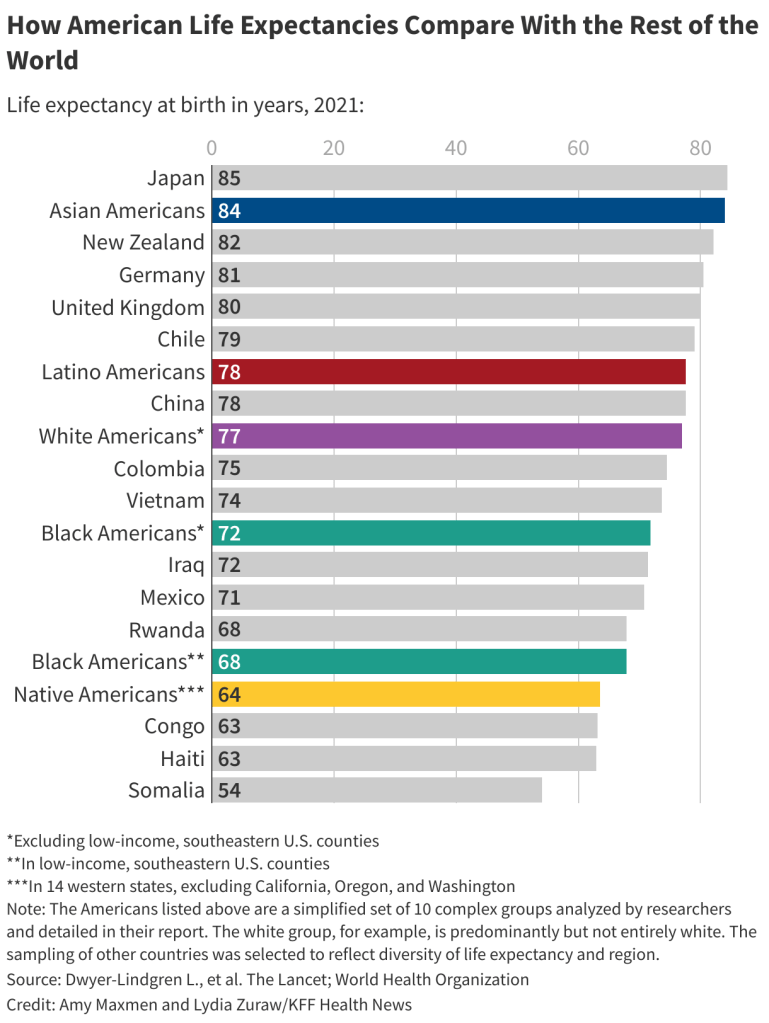
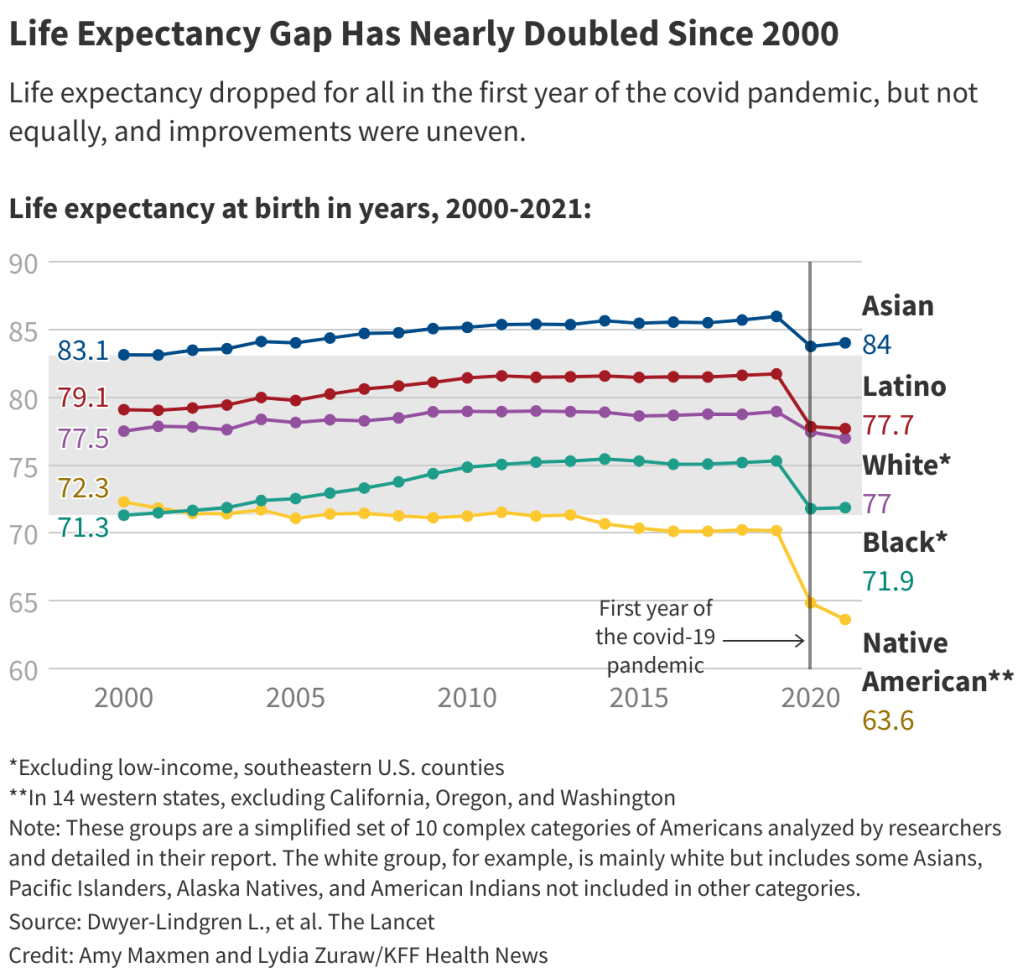
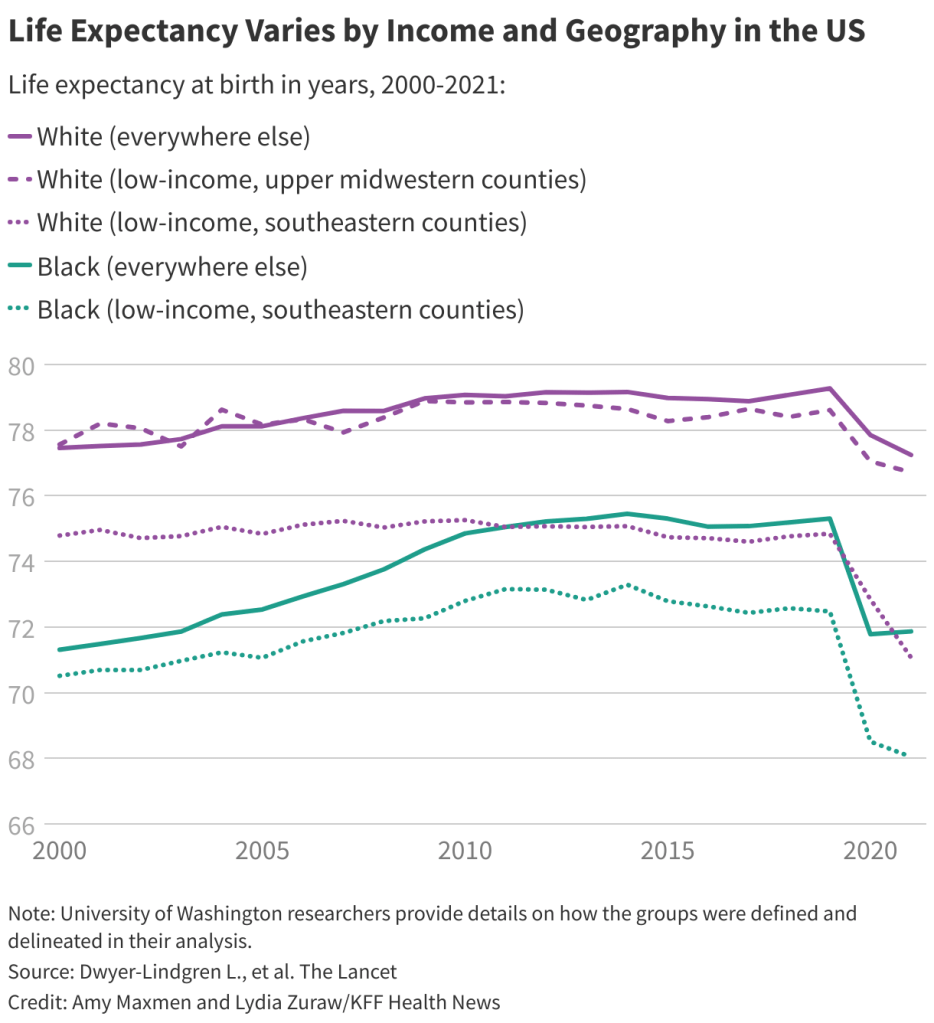
What’s Your America? (there are 10 Americas) – Updated with Scary Charts 02.01.25
Asians and Native Hawaiian or Pacific Islanders definitively outlive other Americans. Is there anything we can learn from them? A confluence of factors may be at play. They tend to have relatively higher socioeconomic status, lower rates of obesity, and the lowest smoking rates of any racial group in the U.S. Healthier traditional cooking may also contribute to their longevity. When it comes to life expectancy, there are 10 Americas – https://bigthink.com/health/ten-americas-for-life-expectancy/
Attention Mortality Risk Experts
Sharpen your pencils and don’t ask me what a pencil is.
Updated 02.01.25 with Scary Charts
More Random Thoughts on Retirement – The Dot Project May 2024
Again, you can’t connect the dots looking forward; you can only connect them looking backward. So you have to trust that the dots will somehow connect in your future. You have to trust in something — your gut, destiny, life, karma, whatever. This approach has never let me down, and it has made all the difference in my life.
Steve Jobs
Let’s be honest: If you keeled over at 68, it would be a family tragedy—but it wouldn’t be a financial one. At that juncture, all your financial problems would be over, and your family would likely be better off financially because they’d inherit your retirement nest egg, which would probably still be largely intact. Instead, the real financial risk is living to a ripe old age. That raises the question: As you make your retirement plans, shouldn’t you care more about the live version of your future self, rather than the dead one?
Long Odds – https://humbledollar.com/2024/05/long-odds/
When I wrote Save as Much as You Can Because Whatever You Manage to Save Will Never Be Enough – Random Thoughts on Retirement I started thinking more about the financial side of living too long. Well, it looks like a ton of media outlets are thinking the same thoughts.
Today’s life expectancies hover just below eighty, and if you reach the milestone of seventy they jump to the mid eighties. Due to advances in medicine and healthier lifestyles, reaching your nineties or even 100 is more realistic than ever. How do you ensure that you don’t run out of money? The answer is to start saving more now and plan to work longer. You’re Going to Live Past 90. Congrats! Here’s How to Pay For It. — https://www.esquire.com/news-politics/a60647995/how-to-afford-living-to-100/
A Big Dot
A little over four and a half years ago at the tender age of 65 my boss asked me if I was planning on retiring or if I wanted to continue working. I said I wanted to continue working. My FRA (full retirement age) for social security retirement benefits was still nearly a year away and I really didn’t want to collect a reduced benefit. As I connect the dots this decision turned out to be a Big Dot. Covid happened. Then inflation soared and continues to soar making everything cost more. I’m glad I didn’t retire back then and lock in a lower monthly lifetime benefit before the cost of everything went up.
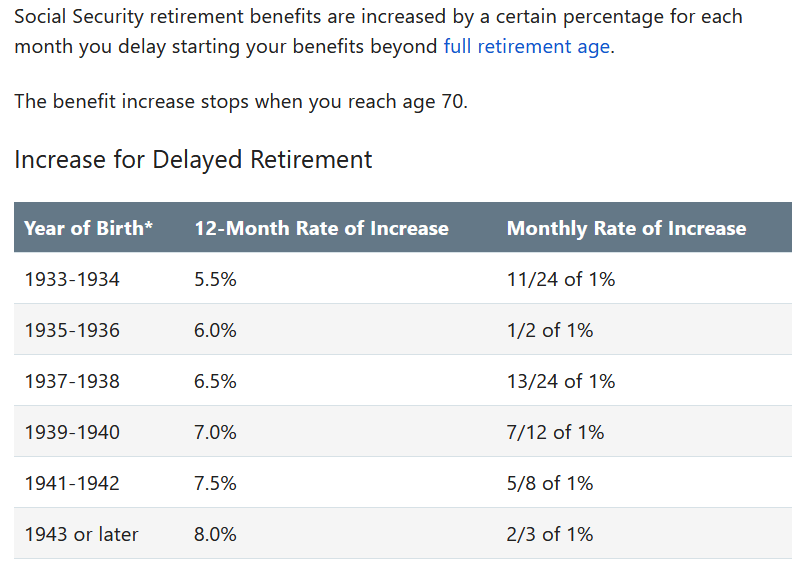
Sometimes things in life work out as planned. Sometimes they don’t. When I decided to stay in the workforce the strategy was to wait until age 70 to collect social security benefits. The math was compelling.
https://www.ssa.gov/benefits/retirement/planner/delayret.html
My focus was simple. All I had to do was stay healthy and stay connected with an employer willing to keep an Old Guy with a particular set of skills on the payroll.
The Road to 70 is now just a short trip. Just 10% of people in one survey planned to wait until age 70 to claim Social Security – https://www.cnbc.com/2023/08/08/survey-just-10percent-plan-to-wait-until-age-70-to-claim-social-security.html. Time for another Big Dot related to this Big Dot. I think I’ll keep working for another 3-5 years, contingent upon the same variables of sustained good health and a willing employer. I have about another 30 years to go, so why not do a few more years of work?
What to Expect as You Age
Rosanne M. Leipzig is a geriatrician and author of the book, Honest Aging: An Insider’s Guide to the Second Half of Life. An earlier post Unlocking the Secrets to Aging Well pointed to a podcast. The following is an excerpt from an article by Judith Graham at KFF Health News titled Let’s Have an Honest Conversation About What to Expect as You Age https://kffhealthnews.org/news/article/navigating-aging-expectation-adjustment-change/. Graham interviewed Dr. Leipzig for the story.
Can the stages of aging be broken down, roughly, by decade? No, said Leipzig, noting that people in their 60s and 70s vary significantly in health and functioning. Typically, predictable changes associated with aging “start to happen much more between the ages of 75 and 85,” she told me. Here are a few of the age-related issues she highlights in her book:
- Older adults often present with different symptoms when they become ill. For instance, a senior having a heart attack may be short of breath or confused, rather than report chest pain. Similarly, an older person with pneumonia may fall or have little appetite instead of having a fever and cough.
- Older adults react differently to medications. Because of changes in body composition and liver, kidney, and gut function, older adults are more sensitive to medications than younger people and often need lower doses. This includes medications that someone may have taken for years. It also applies to alcohol.
- Older adults have reduced energy reserves. With advancing age, hearts become less efficient, lungs transfer less oxygen to the blood, more protein is needed for muscle synthesis, and muscle mass and strength decrease. The result: Older people generate less energy even as they need more energy to perform everyday tasks.
- Hunger and thirst decline. People’s senses of taste and smell diminish, lessening food’s appeal. Loss of appetite becomes more common, and seniors tend to feel full after eating less food. The risk of dehydration increases.
- Cognition slows. Older adults process information more slowly and work harder to learn new information. Multitasking becomes more difficult, and reaction times grow slower. Problems finding words, especially nouns, are typical. Cognitive changes related to medications and illness are more frequent.
- The musculoskeletal system is less flexible. Spines shorten as the discs that separate the vertebrae become harder and more compressed; older adults typically lose 1 to 3 inches in height as this happens. Balance is compromised because of changes in the inner ear, the brain, and the vestibular system (a complex system that regulates balance and a person’s sense of orientation in space). Muscles weaken in the legs, hips, and buttocks, and range of motion in joints contracts. Tendons and ligaments aren’t as strong, and falls and fractures are more frequent as bones become more brittle.
- Eyesight and hearing change. Older adults need much more light to read than younger people. It’s harder for them to see the outlines of objects or distinguish between similar colors as color and contrast perception diminishes. With changes to the cornea, lens, and fluid within the eye, it takes longer to adjust to sunlight as well as darkness.
- Because of accumulated damage to hair cells in the inner ear, it’s harder to hear, especially at high frequencies. It’s also harder to understand speech that’s rapid and loaded with information or that occurs in noisy environments.
- Sleep becomes fragmented. It takes longer for older adults to fall asleep, and they sleep more lightly, awakening more in the night.
This is by no means a complete list of physiological changes that occur as we grow older.
Ouch.

Treatment Resistant Geriatric Depression
Diabesity
Strong, consistent evidence shows that managing obesity can delay progression of prediabetes to type 2 diabetes. Obesity management is also highly beneficial in treating type 2 diabetes, based on the degree of weight loss achieved. Losing excess weight improves glycemic control, reduces the need for glucose-lowering medications, can substantially reduce A1C, and can even promote sustained diabetes remission.
Diabesity Clin Diabetes 2022;40(4):392–393 — https://doi.org/10.2337/cd22-0088
SIDD, SIRD, MOD, AND MARD – DM2 Subgroups
Type 2 diabetes (T2D) was recently reclassified into severe insulin-deficient diabetes (SIDD), severe insulin-resistant diabetes (SIRD), mild obesity-related diabetes (MOD), and mild age-related diabetes (MARD), which have different risk of complications. We explored whether DNA methylation differs between these subgroups and whether subgroup-unique methylation risk scores (MRSs) predict diabetic complications.
Novel Subgroups of Type 2 Diabetes Display Different Epigenetic Patterns That Associate With Future Diabetic Complications — https://doi.org/10.2337/dc21-2489
More acronyms!
Just Another Hump Day…Sweet
Scientists have demonstrated that normal brain aging is accelerated by approximately 26% in people with progressive type 2 diabetes compared with individuals without the disease.
eLife. “Type 2 diabetes accelerates brain aging and cognitive decline.” ScienceDaily. http://www.sciencedaily.com/releases/2022/05/220525080527.htm (accessed May 25, 2022)
Makes you wonder if improving your diet will help.
Many adults can achieve remission of type 2 diabetes with a primary intervention consisting of a diet that emphasizes whole, plant-based foods, according to a new publication from the American College of Lifestyle Medicine (ACLM).
Experts Endorse Plant-Based Diet for Type 2 Diabetes Remission — https://www.medscape.com/viewarticle/974591?src=rss#vp_1
But we all know how hard lifestyle changes can be. Maybe best to just listen to some music.
Combination of biomarkers can identify common cognitive disease — Health Secrets of a SuperAger

In recent years, subcortical small-vessel disease has become an increasingly common cognitive diagnosis. Researchers at University of Gothenburg have now shown that it is possible to identify patients with the disease by combining two biomarkers that are measured in spinal fluid and blood, increasing the potential for both treatment and development of medication. Photo by […]
Combination of biomarkers can identify common cognitive disease — Health Secrets of a SuperAger
I found a blogger who is older than me.
Hell yeah I’m gonna follow him.
Stay as Thin as You Can as Long as You Can
Based on the evidence from clinical trials weight loss (typically 15 kg or greater) is the main driver and predictor of remission.
Dietary strategies for remission of type 2 diabetes: A narrative review — https://doi.org/10.1111/jhn.12938
A weight loss program can lead to type 2 diabetes remission, even in individuals with a normal body mass index (BMI), via loss of body fat, particularly in the liver and pancreas, shows a UK study.
Type 2 Diabetes Remission Possible For Those With Lower BMI — https://www.medscape.com/viewarticle/971599?src=rss#vp_1
The title of this post is a direct quote from an Endocrinologist who at the time was practicing in Dallas Texas. I asked if he had any advice for me to reduce my risk of developing diabetes.
“Stay as thin as you can as long as you can.”
These words have stuck with me ever since.



You must be logged in to post a comment.