Conclusions and Relevance Adults 75 years of age or older with adenoma at prior colonoscopy were more likely to experience subsequent CRC and CRC death compared with those without adenoma, but cumulative risks were low and were far exceeded by competing risks for non-CRC death. Older adults may consider deprioritizing surveillance colonoscopy relative to other health concerns. Colorectal Cancer and Mortality Risk Among Older Adults With vs Without Adenoma on Prior Colonoscopy – https://jamanetwork.com/journals/jama/article-abstract/2847311
older age
(Less Than) Random Thoughts on Retirement – 05.03.26
Yes dear reader, yet another post in the never ending series of random thoughts on retirement. https://lifeunderwriter.net/tag/random-thoughts-on-retirement/
Though the traditional retirement age in the U.S. typically falls between 62 and 67, many Americans continue working beyond that point. As of 2024, slightly more than 22% of adults aged 65 and older are still employed, either full-time or part-time. Though the traditional retirement age in the U.S. typically falls between 62 and 67, many Americans continue working beyond that point. As of 2024, slightly more than 22% of adults aged 65 and older are still employed, either full-time or part-time. – https://financebuzz.com/working-in-retirement-data
I’m not the only Old Guy who is still working past age 65.
But despite the fact I’m not the only Old Guy who is still working past age 65 more people are starting retirements earlier than they expected (always have a Plan B and maybe even a Plan C).
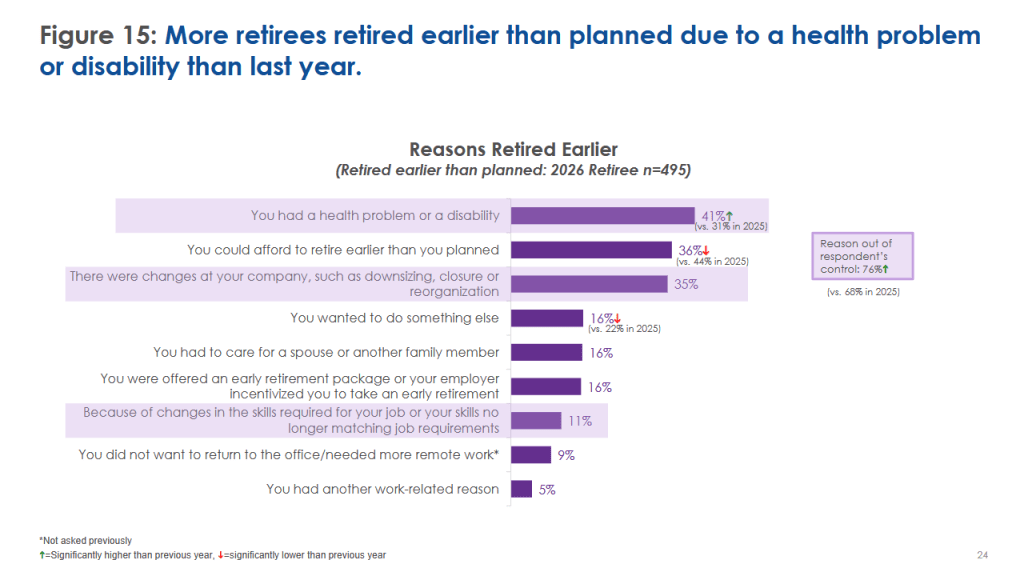
2026 EBRI/Greenwald Retirement Confidence Survey https://www.ebri.org/content/2026-ebri-greenwald-retirement-confidence-survey
I just learned I’m not the only Old Guy who still has a mortgage.
Over the past three decades, the share of homeowners ages 65 to 79 with a mortgage rose from 24% to 41%, while median mortgage debt surged by 400%, according to the Joint Center for Housing Studies at Harvard University. More Americans aging into retirement are still paying down mortgages – https://www.marketplace.org/story/2025/06/09/more-older-americans-continue-to-pay-mortgages
I also learned about the disappearance of structured cognitive demand in retirement.
A 2025 systematic review published in Health Psychology Review found that retirement is associated with measurable cognitive decline, not just because people age, but because structured cognitive demand disappears. Researchers have called it “mental retirement”: The brain follows the body’s example and withdraws from challenge. Gary Has a Plan for Retirement: Crash on the Sofa and Veg. Here’s the Problem With That …https://www.kiplinger.com/retirement/retirement-planning/your-long-term-retirement-plan-needs-a-purpose
I’m now paranoid about the disappearance of structured cognitive demand with a mortgage to pay off and too scared to retire.
More Random Thoughts on Retirement – 03.28.26
We plan for the money. We don’t plan for the Monday morning when no one needs you to be anywhere.
Julianne Holt-Lunstad, a professor of psychology and neuroscience at Brigham Young University, published a landmark meta-analysis in 2015 involving over 3.4 million participants. Her finding: social isolation increases the risk of premature death by 26%, and loneliness by 29%. Those numbers rival the health impact of smoking fifteen cigarettes a day. We treat smoking as a public health crisis. We treat retirement loneliness as a personal failing.
Nobody ever tells you that retirement doesn’t just end your career, it ends the only social structure that was generating daily human contact, and that most people don’t realize their workplace was their entire community until the day they leave it – https://vegoutmag.com/lifestyle/j-a-nobody-ever-tells-you-that-retirement-doesnt-just-end-your-career-it-ends-the-only-social-structure-that-was-generating-daily-human-contact-and-that-most-people-dont-realize-their-workplace-was-th/
Yes dear reader, yet another post in the never ending series of random thoughts on retirement. https://lifeunderwriter.net/tag/random-thoughts-on-retirement/
Though the traditional retirement age in the U.S. typically falls between 62 and 67, many Americans continue working beyond that point. As of 2024, slightly more than 22% of adults aged 65 and older are still employed, either full-time or part-time. Though the traditional retirement age in the U.S. typically falls between 62 and 67, many Americans continue working beyond that point. As of 2024, slightly more than 22% of adults aged 65 and older are still employed, either full-time or part-time. – https://financebuzz.com/working-in-retirement-data
So I’m not the only Old Guy who is still working past age 65.
Benefits of Physical Activity in Older Adults
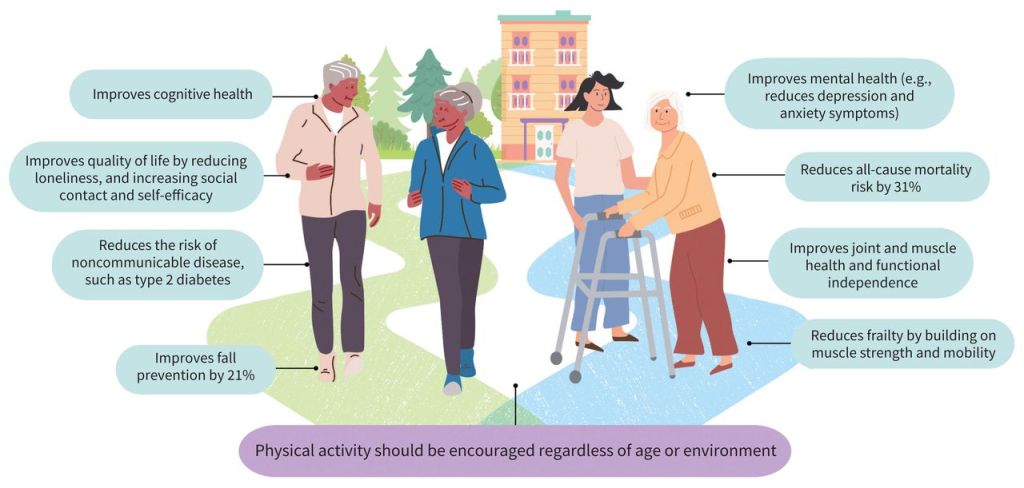
Benefits of physical activity in older adults.
Longevity
The association between physical activity and mortality and morbidity is well established. A 2023 meta-analysis of large prospective studies that examined dose–response found that physical activity levels equivalent to the recommended 150 minutes per week of moderate physical activity reduced all-cause mortality by 31% compared with no physical activity.12 The authors used metabolic equivalent of task (MET), the ratio of work metabolic rate to resting metabolic rate. One MET is equivalent to the energy cost of sitting quietly. A 2019 systematic review and meta-analysis found that, among middle-aged and older adults (aged ≥ 40 yr), higher levels of total physical activity were associated with reduced risk of death in a dose–response relation, such that the most, second-most, and third-most active quartiles were associated with 0.47, 0.35, and 0.28 hazard ratios, respectively, compared with the least active quartile.13 According to a large 2019 observational study, resistance exercise is also associated with reduced mortality independent of aerobic exercise.14 Two 2022 meta-analyses found, respectively, that 60 minutes of resistance exercise per week is associated with a risk reduction of 27% in all-cause mortality15 and that muscle-strengthening activities for 30–60 minutes per week is associated with a 10%–20% reduction.16
Cardiorespiratory fitness and peak exercise capacity are associated with mortality. Peak exercise capacity is a better indicator of risk of death than established cardiovascular risk factors such as smoking, hypertension, and diabetes mellitus.17 A study examining cardiorespiratory fitness in older adults found dose-dependent reductions in mortality across all age groups (including participants aged 60–69, 70–79, and 80–95 yr).18 Substantial improvements (approximately 16%) in VO2max (an individual’s maximum rate of oxygen consumption, a strong indicator of mortality19) in older adults can occur with only 90 minutes of submaximal exercise per week over 16–20 weeks.20
Strength is also associated with reductions in all-cause mortality in older adults. A 2022 systematic review and meta-analysis found a linear inverse relation between handgrip strength and all-cause mortality up to sex-dependent thresholds (42 kg for men, 25 kg for women) in older adults.21 In their 2018 systematic review and meta-analysis, the authors found both handgrip and knee extension strength to be predictors of all-cause mortality in adults, with most of the studies examining adults older than 65 years.22 – Move more, age well: prescribing physical activity for older adults CMAJ January 27, 2025 197 (3) E59-E67; DOI: https://doi.org/10.1503/cmaj.231336
The Best Resistance Training Program
A key takeaway from the updated guidelines is that the biggest benefits often come from a simple starting point. Transitioning from no resistance training to any regular activity can lead to meaningful improvements. While factors such as load, volume, and frequency can be adjusted, experts say the main priority for most adults should be building a routine they can follow consistently.
Another important shift in the recommendations is the recognition that effective resistance training does not require access to a gym. Exercises using elastic bands, bodyweight movements, or simple at home routines can still produce measurable gains in strength, muscle size, and daily function. McMaster University. “The best strength training plan might be simpler than you think.” ScienceDaily https://www.sciencedaily.com/releases/2026/03/260319074552.htm
Source: https://acsm.org/resistance-training-guidelines-update-2026/
Resistance is not futile.
The Nutritional Challenges of Advanced Age
The study focused exclusively on adults 80 and older, a group with very different dietary requirements than younger adults. As people age, the body goes through significant physiological changes. Energy expenditure decreases, and losses in muscle mass, bone density, and appetite are common. Together, these changes increase the risk of malnutrition and frailty.
Most evidence for the health benefits of diets that exclude meat comes from studies of younger adults rather than frail older populations. Some research suggests older non-meat eaters face a higher risk of fractures due to lower calcium and protein intake.
In later life, nutritional priorities shift. Rather than focusing on preventing long-term diseases, the goal becomes maintaining muscle mass, preventing weight loss and ensuring every mouthful delivers plenty of nutrients. Study finds vegetarians over 80 less likely to reach 100 -The Conversation. https://www.sciencedaily.com/releases/2026/02/260225081214.htm “Study finds vegetarians over 80 less likely to reach 100.” ScienceDaily. (accessed February 27, 2026).
Story Source:
Materials provided by The Conversation. Original written by Chloe Casey, Lecturer in Nutrition and Behaviour, Bournemouth University. Note: Content may be edited for style and length.
Keep Moving
Physical activity consistently emerges as the most important factor influencing both absolute physical capacity and the rate of age-related decline. Our longitudinal data are consistent with previous studies showing that regular physical activity can attenuate the decline in physical performance [17, 32–37]. Individuals who were physically active in their leisure time at age 16 maintained higher aerobic capacity, muscular endurance and muscle power throughout the observation period. This emphasizes the importance of early intervention to establish positive exercise habits in adolescence and early adulthood, as these patterns appear to have long-term benefits for physical function. Encouragingly, our results show that transitioning from physical inactivity to activity at any age significantly improves performance in all fitness modalities studied. These findings contradict the assumption that early inactivity irreversibly impairs physical performance. Rather, taking up regular physical activity leads to measurable improvements in performance even in later decades of life. This finding is of particular importance for clinical practice, as physical activity is still the only evidence-based intervention to reduce the risk of sarcopenia [2, 38]. Recent large population studies also show that an active lifestyle is beneficial at any age [13, 39, 40]. Rise and Fall of Physical Capacity in a General Population: A 47-Year Longitudinal Study – https://onlinelibrary.wiley.com/doi/10.1002/jcsm.70134
Text above in bold are my highlights.
Despite the documented limitations this is a very strong study.
I’ve been doing my home based virtual physical therapy for nearly a year. I’m trying to get to the gym at least twice a week. I don’t walk as much as I used to but…
Keep moving.
Random Thoughts on Unretirement – 01.10.26
“We have to understand that anything in the past takes you out of the present moment. Anything in the future takes you out of the present moment.”
Zen Master Daigneault
To readers who are visiting this blog for the first time my posts on Random Thoughts About Retirement and Unretirement are written by an Old Guy who is old enough to be retired but isn’t retired and is still working. I had another birthday and the older I get the more I think about retirement. Back in 2023 I was thinking about what retirement for me would look like (see More Random Thoughts on Retirement – June 2023). But decisions such as this take serious thought and consideration. At first I thought I wanted to retire to a quiet life of blogging and writing my Future Best Seller titled The Man Who Had No Hobbies. After much thought I decided to add a short term goal to my retirement plan. My new short term goal is to avoid unretirement.
My RSS feed feeds me headlines on unretirement.
According to a new report from T. Rowe Price around 7% of retirees are looking for work in retirement, while 20% say they’re already working part time or full time…The two main reasons for coming back into the workforce are a tale of opposites. While 45% chose to work for social and emotional benefits… a slightly larger percentage — 48% — felt they needed to work for financial reasons.
Unretiring: More retirees are going back to work because they want to — or need to — https://finance.yahoo.com/news/unretiring-more-retirees-are-going-back-to-work-because-they-want-to–or-need-to-123203300.html
And this.
Once an eagerly awaited milestone, retirement is currently undergoing a transformative reevaluation. Traditionally seen as a well-deserved period of rest and relaxation, the dream of early retirement is now being challenged by a new perspective – that of embracing lifelong work. This paradigm shift reflects the changing nature of work, increased life expectancy, and the desire for personal fulfillment.
Rethinking Retirement: The Case for Embracing Lifelong Work — https://due.com/rethinking-retirement-the-case-for-embracing-lifelong-work/
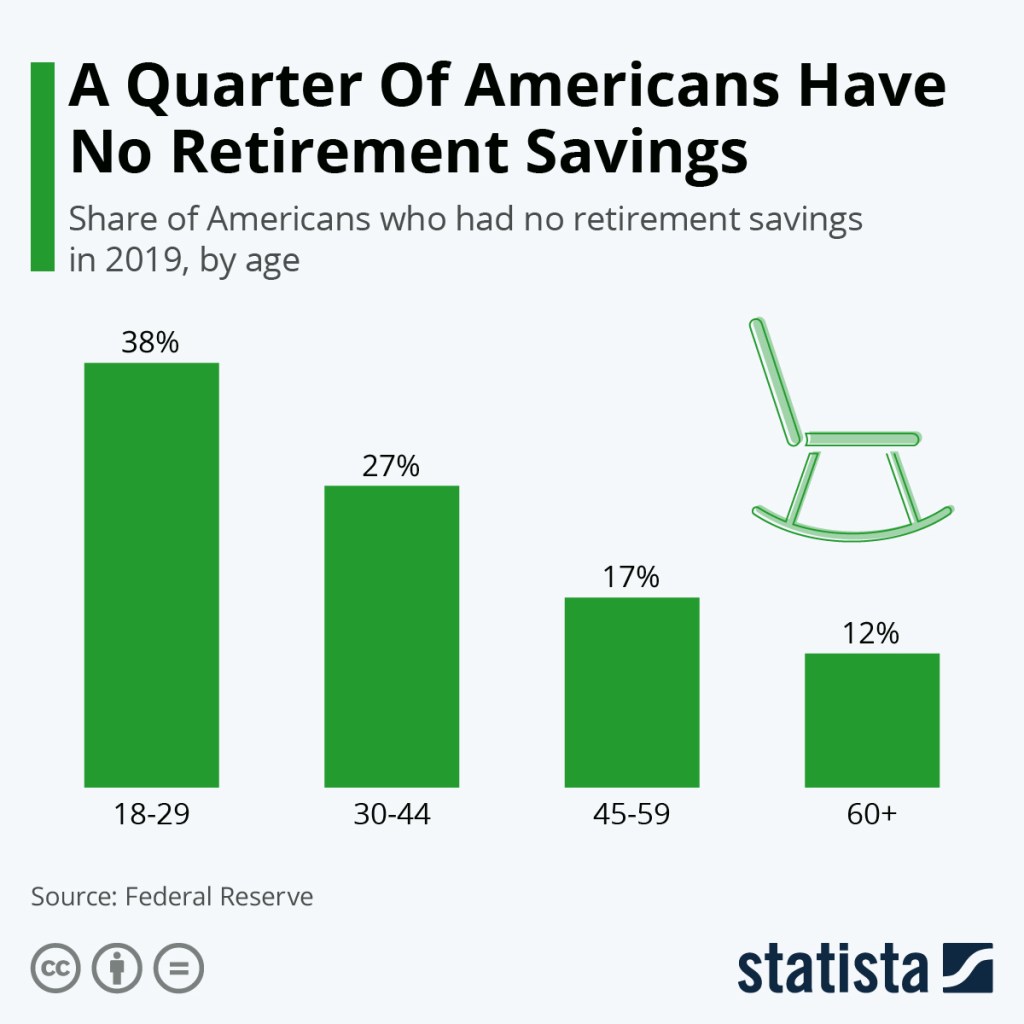
The reality is many won’t have a choice. The following chart illustrates retirement savings as of 2019.
Americans are having trouble financially preparing themselves for life after work. A recent Federal Reserve report found that nearly a quarter of U.S. adults have absolutely no retirement savings or pension. Even though the level of preparation increases as people get older, concern about inadequate savings is still readily apparent across all age groups, even older people in their 60s.
A Quarter Of Americans Have No Retirement Savings — https://www.statista.com/chart/18246/share-of-americans-who-have-no-retirement-savings/
OOPS. I’m glad I didn’t click the Publish button. The savings situation appears to be worse than I thought. The study below was an analysis of data from 2010!
The study broadly examines how American households are faring in relation to retirement savings targets recommended by some financial services firms. It uses the Federal Reserve’s Survey of Consumer Finances to analyze retirement plan participation, savings, and overall assets of all U.S. households age 25 to 64, not just those with retirement account assets. This is important because some 45 percent, or 38 million working-age households, do not have any retirement account assets.
The average working household has virtually no retirement savings. When all households are included— not just households with retirement accounts—the median retirement account balance is $3,000 for all working-age households and $12,000 for near-retirement households. Two-thirds of working households age 55-64 with at least one earner have retirement savings less than one times their annual income, which is far below what they will need to maintain their standard of living in retirement.
The findings confirm that the American Dream of retiring comfortably after a lifetime of work will be impossible for many. Based on 401(k)–type account and IRA balances alone, some 92 percent of working households do not meet conservative retirement savings targets for their age and income. Even when counting their entire net worth, 65 percent still fall short.
The Retirement Savings Crisis: Is It Worse Than We Think? — https://www.nirsonline.org/reports/the-retirement-savings-crisis-is-it-worse-than-we-think/
So how will you afford retirement without any savings? Don’t look to Social Security. Here’s some numbers on average Social Security payments. The full chart at the source website goes up to age 100.
As of December 31, 2021, the average Social Security payment for all retirees was $1,658.03 a month, according to the Social Security Administration’s Annual Statistical Supplement for 2022. For men, the overall average was $1,838.08. For women, the average was $1,483.75 — a difference of $354.33 per month.
Here’s the Average Social Security Check for Men vs. Women — https://www.gobankingrates.com/retirement/social-security/average-social-security-check-men-women/
I’ve previously advised everyone to Save as Much as You Can Because Whatever You Manage to Save Will Never Be Enough – Random Thoughts on Retirement. Now here’s my second piece of sage advice: keep working so you don’t have to unretire.
Whether people unretire or simply stay in the workforce longer, some of the largest financial benefits of additional years of work are delaying retirement account withdrawals and delaying claiming Social Security benefits. These actions essentially shorten the amount of time your assets will need to support you in retirement. Even a few additional years of income have a positive effect on the probability that you won’t outlive your funds.
“Unretiring”: Why Recent Retirees Want to Go Back to Work — https://www.troweprice.com/personal-investing/resources/insights/unretiring-why-recent-retirees-want-to-go-back-to-work.html
Whew. Long post. Longer than I anticipated. If you made it this far, congratulations!
Double OOPS. Hit the publish button too soon. Postscript.
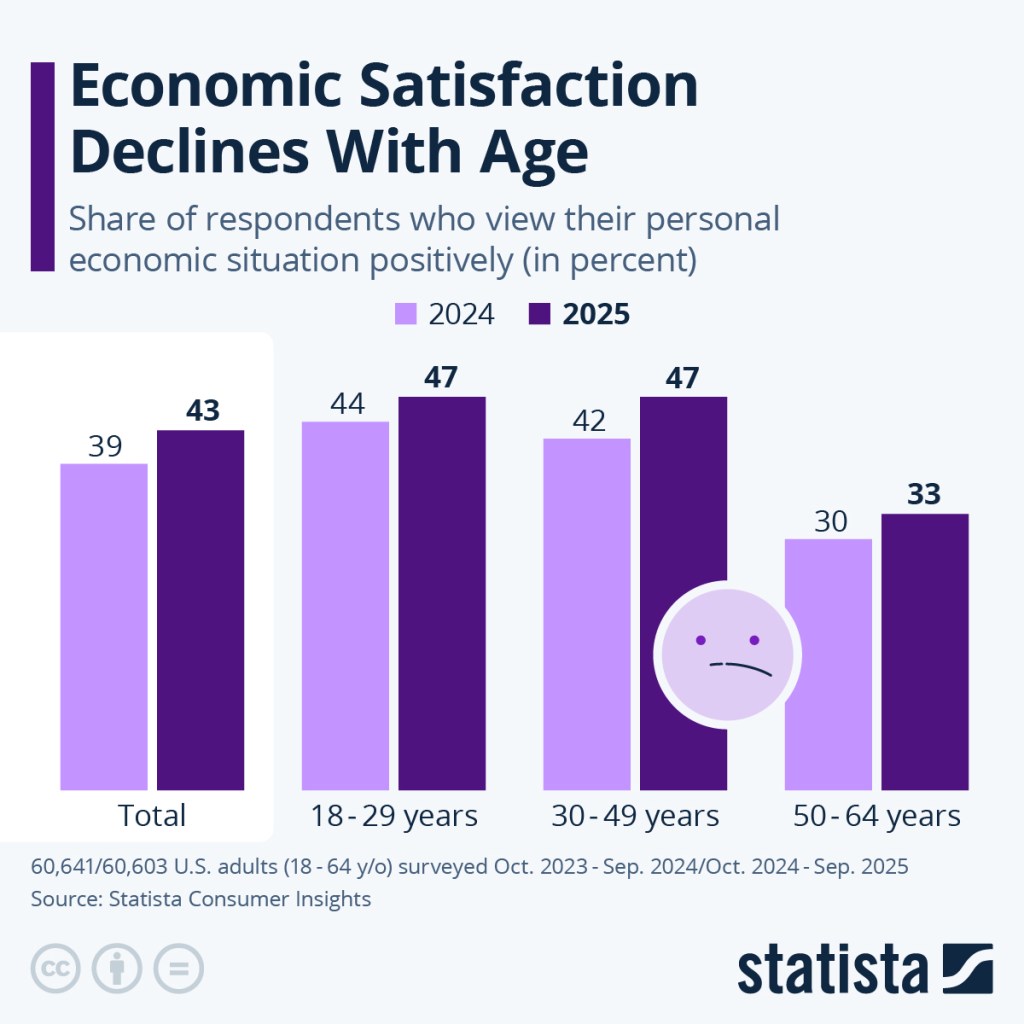
Economic Satisfaction Declines With Age – https://www.statista.com/chart/35656/us-respondents-who-view-their-financial-situation-positively/
Note the survey respondents’ age stops at 64.
Random Thoughts on Retirement (or why I continue to work)
Congress needs to get serious about tweaking various aspects of Social Security, but this time to improve the financial aspects of the system, and not to make them worse, as it had done in January.Social Security Fiscal Year 2025: Trust Fund Balance, Income, Outgo, Deficit, and Interest Rates https://wolfstreet.com/2025/11/18/social-security-fiscal-year-2025-trust-fund-balance-income-outgo-deficit-and-interest-rates/
The Boss (SWMBO) and I talk about this often. Once the W2 income stops and we have to rely upon a small corporate pension, savings, and a shaky Social Security promise we’ll have to get conservative on our spending. No more Stratocasters. Less purchases for wardrobe enhancements. Gas station beer instead of craft brews.
Time will tell.
SWMBO – She Who Must Be Obeyed
Yikes.
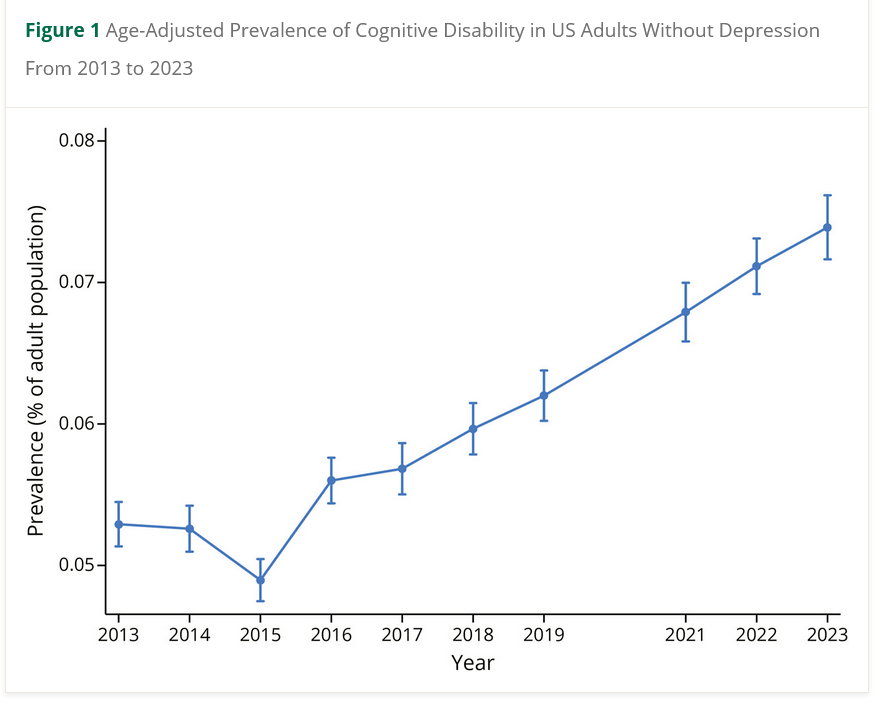
Scary Charts 11.15.25 (income matters)
Cognitive disability was strongly associated with socioeconomic factors such as income and education. Adults with household incomes less than $35,000 consistently reported the highest prevalence, increasing from 8.8% (95% CI 8.5%–9.2%) in 2013 to 12.6% (95% CI 12.0%–13.2%) in 2023. By contrast, adults in the highest income bracket (household income ≥ $75,000) had substantially lower prevalence, with a more modest increase from 1.8% (95% CI 1.6%–2.0%) in 2013 to 3.9% (95% CI 3.6%–4.2%) in 2023. Rising Cognitive Disability as a Public Health Concern Among US Adults – Neurology October 21, 2025 issue 105 (8) e214226 https://doi.org/10.1212/WNL.0000000000214226
Overall, income is central to the aging experience. From how well they think they’re aging to how they rate their physical and mental health and financial security, older adults with upper incomes are doing better than those with middle or lower incomes. Aging well: How income and health shape the experiences of older Americans – https://www.pewresearch.org/social-trends/2025/11/06/aging-well-how-income-and-health-shape-the-experiences-of-older-americans/
Yikes.

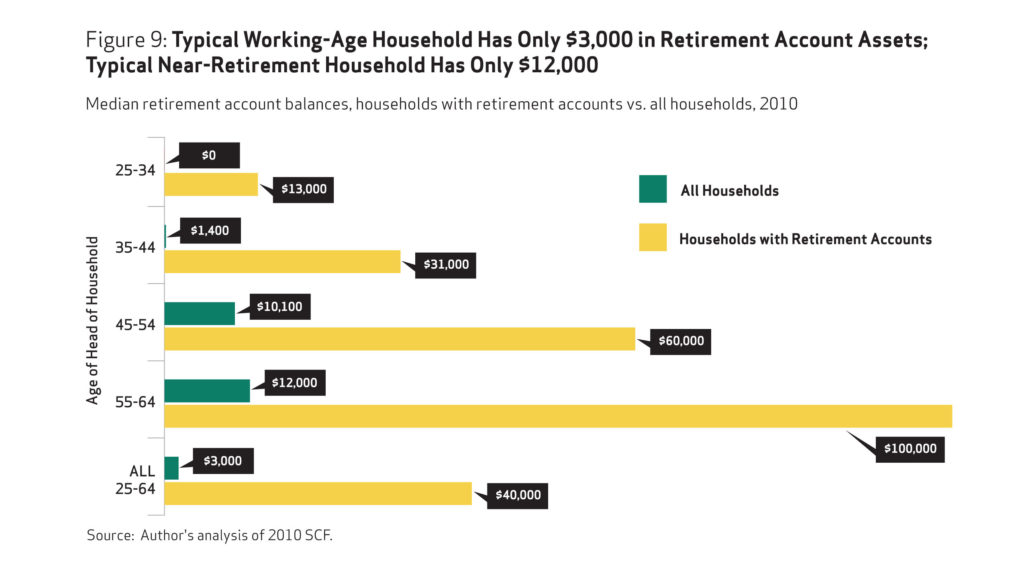
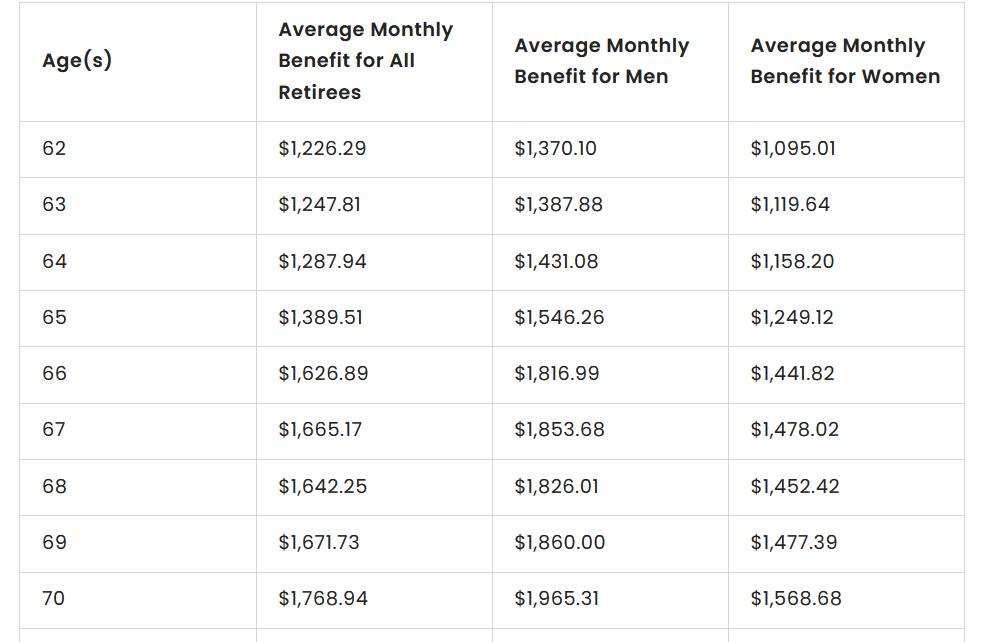



You must be logged in to post a comment.