“We see cases where people take a GLP-1 medication and become so severely malnourished that they need to be hospitalized,” said Rebecca Boswell, PhD, director of Penn Medicine Princeton Center for Eating Disorders, in Philadelphia. “It’s not uncommon.” The Scary Health Risk That Can Sneak Up on GLP-1 Users – Medscape – January 19, 2026. https://www.medscape.com/viewarticle/scary-health-risk-can-sneak-glp-1-users-2026a10001pi
Yikes.
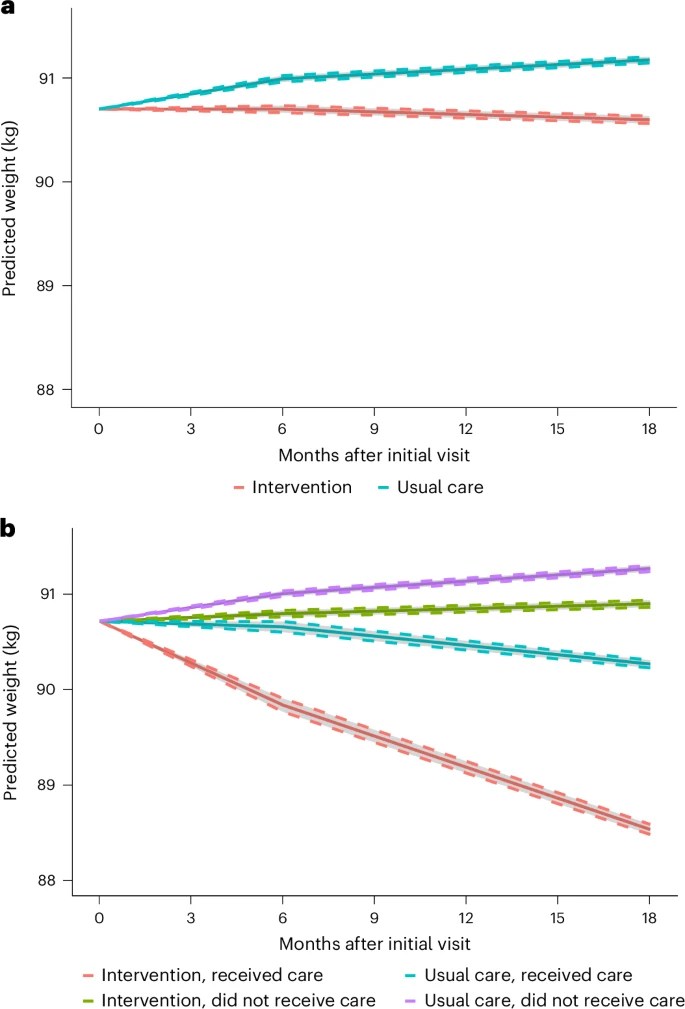
People return to their baseline weight and lose all cardiometabolic benefits in less than 2 years after stopping semaglutide or tirzepatide, a new meta-analysis found. Weight Regain, Health Benefit Loss Rapid When GLP-1s Stopped – Medscape – January 08, 2026. https://www.medscape.com/viewarticle/weight-regain-health-benefit-loss-rapid-when-glp-1s-stopped-2026a10000kr?
YIKES.
You see, cures are passée. Cures kill markets. Getting the population properly hooked on a pharmaceutical treatment for a ‘chronic’ condition is where the serious money is. “Our core insight was simple and grim: it’s far easier—and infinitely more profitable—to convince healthy people that they’re sick than to develop genuine cures for the truly ill.“
Twenty years later, the hustle is bigger, slicker, and more dangerous than ever. Watching that hustle unfold with weight loss drugs feels weirdly ominous, like watching a slow-moving train wreck you can’t peel your eyes off of. You know there’ll be carnage and bodies, vast fortunes won and lost, and humanity left just a little bit poorer. We have often documented the pharmaceutical industry’s proven ability to create enormously lucrative markets overnight, by inventing and selling diseases. Now watch as all that ingenuity and energy gets pointed at one of the biggest problems bewitching humanity: human fatness. The Seven Deadly Sins of Weight Loss Drugs – https://brownstone.org/articles/the-seven-deadly-sins-of-weight-loss-drugs/
YIKES!
This will not end well.
Complications? What Complications? (just another GLP-1 receptor agonist post)
You must be logged in to post a comment.