Conclusions and Relevance Adults 75 years of age or older with adenoma at prior colonoscopy were more likely to experience subsequent CRC and CRC death compared with those without adenoma, but cumulative risks were low and were far exceeded by competing risks for non-CRC death. Older adults may consider deprioritizing surveillance colonoscopy relative to other health concerns. Colorectal Cancer and Mortality Risk Among Older Adults With vs Without Adenoma on Prior Colonoscopy – https://jamanetwork.com/journals/jama/article-abstract/2847311
Understanding Medical Technologies
America’s Largest Hospital System Ready to Start Replacing Radiologists With AI
“We could replace a great deal of radiologists with AI at this moment, if we are ready to do the regulatory challenge,”
Mitchell Katz, president and CEO of New York’s 11-hospital public benefit corporationMohammed Suhail, a radiologist at North Coast Imaging in San Diego, told Radiology that Katz’s comments are “undeniable proof that confidently uninformed hospital administrators are a danger to patients (and are) ..“easily duped by AI companies that are nowhere near capable of providing patient care.”
America’s Largest Hospital System Ready to Start Replacing Radiologists With AI, Its CEO Says – https://futurism.com/artificial-intelligence/hospital-ceo-ai-radiology
Confidently. Uninformed.
Yikes.
Underlying Causes and Causal Pathways are Largely Unknown (guess the disease)
Using high-quality population-based cancer registry data until 2017, this study presents contemporary trends in early-onset colorectal cancer incidence across 50 countries and territories, including 12 additional countries (Argentina, Bahrain, Belarus, Chile, Columbia, Ecuador, France [Martinique], Iceland, Kuwait, the USA [Puerto Rico], Qatar, and Uganda) since the last published report on colorectal cancer incidence trends. The findings show that the rising incidence of early-onset colorectal cancer is no longer limited to high-income countries; it now extends to countries and territories in Latin America and the Caribbean (Argentina, Chile, Costa Rica, Ecuador, Martinique, and Puerto Rico), Asia (Israel, Japan, Thailand, and Türkiye), and eastern Europe (Belarus). Colorectal cancer incidence trends in younger versus older adults: an analysis of population-based cancer registry data – https://www.thelancet.com/journals/lanonc/article/PIIS1470-2045(24)00600-4/fulltext
Yikes.
Brugada Syndrome
A 36-year-old female presents to the ED after experiencing an episode of sudden syncope. The patient has no significant past medical history, and reports that she was walking to the end of her driveway to retrieve her mail when she suddenly collapsed to the ground. She recalls waking up on her driveway with concerned neighbors gathered around her…
http://www.emdocs.net/em3am-brugada-syndrome/
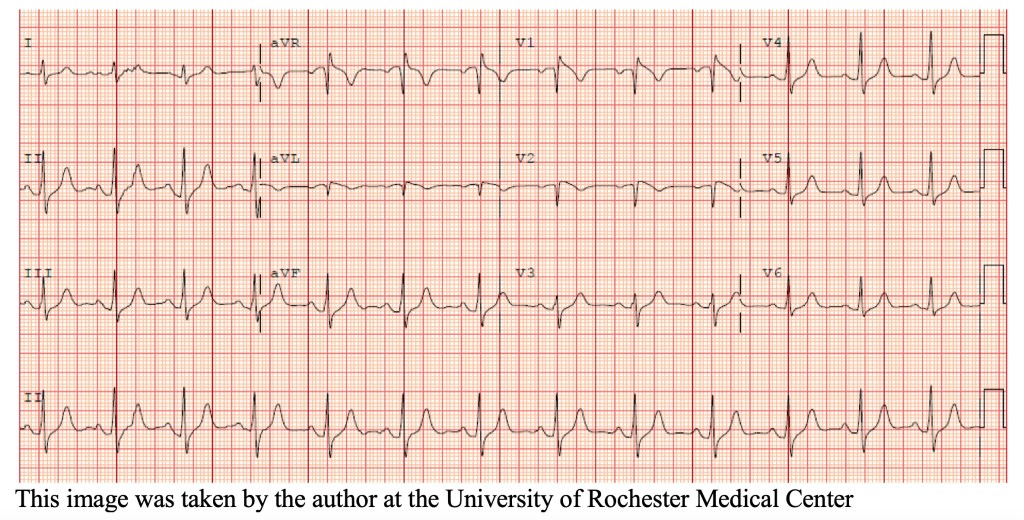
Dear Readers – another Saturday morning and this Grandpa Underwriter is back to his old tricks of reading about things that are WAY ABOVE his pay grade. There are two clinical scenarios in the article. Enjoy!
Emphysema More Common in Marijuana Smokers Than Cigarette Smokers
“We know what cigarettes do to the lungs,” said study author Giselle Revah, M.D., a cardiothoracic radiologist and assistant professor at the University of Ottawa in Ottawa, Canada. “There are well researched and established findings of cigarette smoking on the lungs. Marijuana we know very little about.”
To find out more, Dr. Revah and colleagues compared chest CT results from 56 marijuana smokers with those of 57 non-smoking controls and 33 tobacco-only smokers.
Three-quarters of the marijuana smokers had emphysema, a lung disease that causes difficulty with breathing, compared with 67% of the tobacco-only smokers. Only 5% of the non-smokers had emphysema. Paraseptal emphysema, which damages the tiny ducts that connect to the air sacs in the lungs, was the predominant emphysema subtype in marijuana smokers compared to the tobacco-only group.
Radiological Society of North America. “Emphysema more common in marijuana smokers than cigarette smokers.” ScienceDaily. http://www.sciencedaily.com/releases/2022/11/221115113940.htm (originally accessed November 15, 2022).
Journal Reference
Luke Murtha, Paul Sathiadoss, Jean-Paul Salameh, Matthew D. F. Mcinnes, Giselle Revah. Chest CT Findings in Marijuana Smokers. Radiology, 2022; DOI: 10.1148/radiol.212611
The mean age of the MJ smokers in the study was 49.
The mean age of the tobacco smokers in the study was 60.

This Wearable Ultrasound Sticker Can Continuously Image Organs for 48 Hours – smithsonianmag.com
Developed by engineers at MIT, the new technology is about the size of a postage stamp
This Wearable Ultrasound Sticker Can Continuously Image Organs for 48 Hours — Latest articles | smithsonianmag.com
Memo to Self – 03.18.22
Stuff I Wish I Had When Starting My Career
Colonoscopy – Just Do It (an almost forgotten post)
I came across this post in my collection of unpublished drafts. I thought I posted this but obviously I didn’t. This article link was intended to be posted before Colorectal Cancer Rates Rising in Ages 50-54. Better late than never, I guess.
More than one quarter of colonoscopies carried out in Americans aged 30 to 49 years reveal some type of neoplasm, and slightly over 6% of these patients have advanced cancer, results of a nationally representative endoscopic registry show.
One Quarter of 30–49-Year-Olds Have Abnormal Colonoscopy Results – Medscape – Jun 07, 2021. — https://www.medscape.com/viewarticle/952536?src=rss#vp_1

Also see Study Finds Sharp Rise in Colon Cancer and Rectal Cancer Rates Among Young Adults and Diet and Colon Cancer Risk – CBS News.
Colorectal Cancer Rates Rising in Ages 50-54
During the period 1992–2018, there were a total of 101,609 cases of CRC among adults aged 45–59 years. Further analysis showed that the CRC incidence rates rose from 23.4 to 34.0 per 100,000 among people aged 45–49 years and from 46.4 to 63.8 per 100,000 among those aged 50–54 years. Conversely, incidence rates decreased among individuals aged 55–59 years, from 81.7 to 63.7 per 100,000 persons.
Colorectal Cancer Rates Rising in People Aged 50 to 54 Years – Medscape – Nov 11, 2021 – https://www.medscape.com/viewarticle/962769?src=rss#vp_2
I am posting a link to this article as I enjoy the effects of 238 grams of Miralax mixed with a gallon of sports beverage and/or water. It certainly takes your mind off of not eating all day.
You must be logged in to post a comment.